Aviva has disclosed it paid out a total of £128m ($159m) in private medical claims due to COVID-19. This highlights the scale of damage to the industry caused by the pandemic and its fallout. The insurer said it has made its last COVID-related payout, meaning this is its final claims figure.
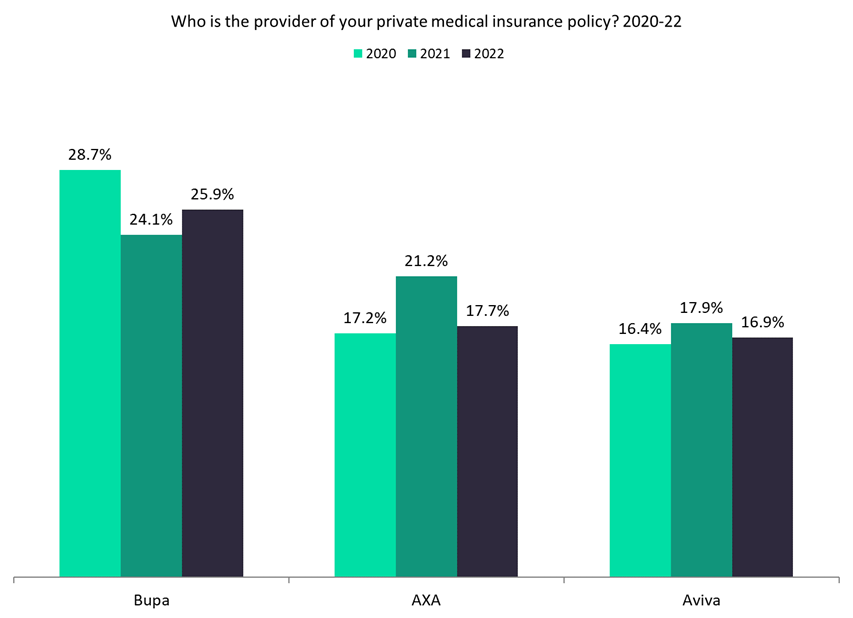
GlobalData findings show that Aviva was the third-largest private medical insurer in the UK in 2022 (a position it also held in 2020 and 2021) with 16.9% of the market. In 2022, it was behind only Bupa (25.9%) and AXA (17.7%) – both of which likely suffered even higher claims due to the pandemic. Aviva announced it paid out a further £47m in claims in May 2023, bringing its total to £128m.
As per GlobalData’s UK Top 20 General Insurance Competitor Analytics, total medical expenses premiums were £5.3bn in 2021 (the latest data available), which suggests Aviva receives around £800m in premiums each year. This shows that while COVID-19 has not been devastating for Aviva, it still faced significant payouts comparative to its premiums. This may have been somewhat alleviated by fewer health-related claims for other ailments over this period due to lockdowns and restrictions in the UK.
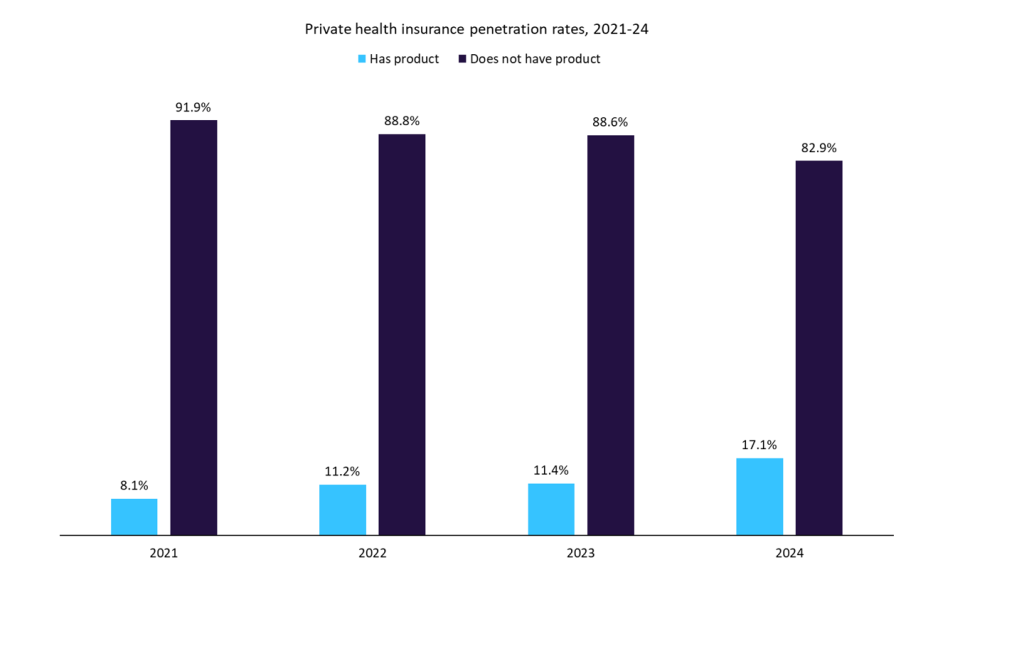
The hope for the insurer is that a global pandemic will have alerted more people to the importance of private medical insurance. This should lead to an increase in penetration rates and subsequently premiums. In addition, GlobalData’s 2022 UK Insurance Consumer Survey found that NHS waiting lists were the key trigger cited by individuals purchasing private medical insurance (27%). COVID-19 had a significant impact on NHS waiting lists and is therefore likely to have encouraged more people to take out a policy.
How well do you really know your competitors?
Access the most comprehensive Company Profiles on the market, powered by GlobalData. Save hours of research. Gain competitive edge.

Thank you!
Your download email will arrive shortly
Not ready to buy yet? Download a free sample
We are confident about the unique quality of our Company Profiles. However, we want you to make the most beneficial decision for your business, so we offer a free sample that you can download by submitting the below form
By GlobalData




Related Company Profiles
AXA SA
Aviva Plc